What about treatment of asymptomatic carotid artery disease?
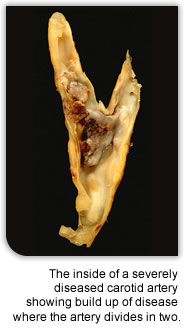 Some people will, for one reason or another, have a scan that shows that they have narrowing of the carotid arteries even though they have never had any symptoms. The question arises as to what to do about it? The first and most important point is that if you are found to have narrowing of the carotid arteries this suggests that there are factors at work which make you prone to furring up of your arteries. In general furring up of the arteries (atherosclerosis) is a problem that affects all the arteries to some degree so that if the neck arteries are being furred up there is an increased risk of furring up of the heart arteries or the leg arteries. It is therefore sensible to look at all the things which may be making you more prone to furring up the arteries and see what can be done about them. The risk factors are smoking, high blood pressure, diabetes, high cholesterol and family history. Some of these can be dealt with and some of them cannot but it is important to do everything possible to minimise the risk of worsening arterial disease and try and prevent any further arterial disease developing in future. You should discuss this with your GP. So the first thing to do is to deal with the risk factors. However, the question remains as to what, if anything, should be done about the narrowed carotid artery? There is some debate about this. There are some good randomised controlled studies in which patients with carotid artery disease of which half had surgery and half did not. The risk of stroke is reduced by about 50% in those who do have surgery compared with those who do not. However, while this sounds impressive, the actual risk of having a stroke in the first place is far lower in someone who has never had any symptoms from their narrowed artery than in those who have had symptoms. This is because, as explained above, furring up of the artery may often not cause any symptoms whatsoever and usually it is when the artery becomes unstable that the symptoms and the stroke can arise. Many people with narrowing of the carotid arteries will never get any instability of the artery and never have a stroke. It follows that you have to treat a lot more arteries to prevent a stroke if they are asymptomatic than if they have caused symptoms. The medical treatment of arterial disease is improving and some people would argue that it is now so good that there is no need for carotid artery surgery or treatment in this group.
Some people will, for one reason or another, have a scan that shows that they have narrowing of the carotid arteries even though they have never had any symptoms. The question arises as to what to do about it? The first and most important point is that if you are found to have narrowing of the carotid arteries this suggests that there are factors at work which make you prone to furring up of your arteries. In general furring up of the arteries (atherosclerosis) is a problem that affects all the arteries to some degree so that if the neck arteries are being furred up there is an increased risk of furring up of the heart arteries or the leg arteries. It is therefore sensible to look at all the things which may be making you more prone to furring up the arteries and see what can be done about them. The risk factors are smoking, high blood pressure, diabetes, high cholesterol and family history. Some of these can be dealt with and some of them cannot but it is important to do everything possible to minimise the risk of worsening arterial disease and try and prevent any further arterial disease developing in future. You should discuss this with your GP. So the first thing to do is to deal with the risk factors. However, the question remains as to what, if anything, should be done about the narrowed carotid artery? There is some debate about this. There are some good randomised controlled studies in which patients with carotid artery disease of which half had surgery and half did not. The risk of stroke is reduced by about 50% in those who do have surgery compared with those who do not. However, while this sounds impressive, the actual risk of having a stroke in the first place is far lower in someone who has never had any symptoms from their narrowed artery than in those who have had symptoms. This is because, as explained above, furring up of the artery may often not cause any symptoms whatsoever and usually it is when the artery becomes unstable that the symptoms and the stroke can arise. Many people with narrowing of the carotid arteries will never get any instability of the artery and never have a stroke. It follows that you have to treat a lot more arteries to prevent a stroke if they are asymptomatic than if they have caused symptoms. The medical treatment of arterial disease is improving and some people would argue that it is now so good that there is no need for carotid artery surgery or treatment in this group.
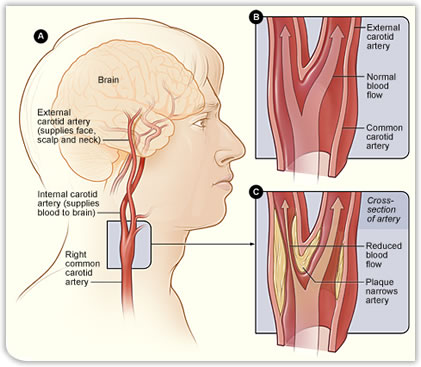
My own view is that there is still a place for carotid intervention in patients with severe asymptomatic carotid disease. However, it is important that patients considered for this should have a good life expectancy because the risks of carotid intervention occur at the time of the procedure whereas the benefits occur in the following years, as the risk of having a stroke with each successive year is lower than it would have been if the operation had not been done. Clearly if somebody has a very short life expectancy they are unlikely to live long enough to see the benefit of the procedure. It is worth remembering that most strokes occur without prior warning and so just relying on warning mini strokes to pick out patients for intervention will only deal with a small part of the problem. The long-term future clearly lies in improving our ability to detect which asymptomatic carotid artery plaques are likely to cause stroke and which can safely be left alone. The key here is to predict which patients with asymptomatic disease are likely to have a stroke and intervene with these patients and avoid the risks and cost of treatment in those who were very unlikely to have a stroke anyway. This has been a major research interest of mine and pioneering work in Nottingham using MRI to detect bleeding inside the narrow carotid artery (intraplaque haemorrhage) is an excellent way of predicting those at risk.